Aeromedical Factors

Medications and the FAA
Obviously, lots of us take medications for one thing or another. If you are training for your Sport Pilot Certificate it is especially important you are familiar with what is and is not allowed by the FAA as you may not be regularly seeing an AME (aviation medical examiner, basically a pilot doctor). Only AMEs are qualified to tell you what you can and cannot take while flying. Regular doctors do not have the same training and expertise as AMEs. For Private Pilots, you still need to be familiar with what is and is not approved by the FAA for you to take. The FAA maintains a good list of meds both allowed and not allowed for pilots on their website. As a private pilot you will have a medical certificate and already have established a relationship with an AME, making it easy for you to call their office and ask questions about any new meds you may be taking.
Just because you get a 3rd class or other medical certificate and it is valid for a certain length of time, if you change the medications you are taking during that time you may not be able to exercise the privileges of that medical certificate. Below you will find a link to one of our articles on what meds are specifically banned by the FAA, and what the length of time is you have to wait to fly after taking those medications. Just because the meds you are taking are not on the “banned” list does not mean they are okay. The only way you can be certain that you can fly with the medications you have taken or are currently taking is to check both the FAA website for allowed medications and check with your AME as well.
Aeromedical Factors
Being that pilots are just people, we are susceptible to a number of physical issues when we expose our bodies to flying. Below we will talk about the most common aeromedical factors a private pilot should be familiar with and know how to remedy or avoid such scenarios. We’ll define each and also give the signs and/or remedy associated with each:
Hypoxia
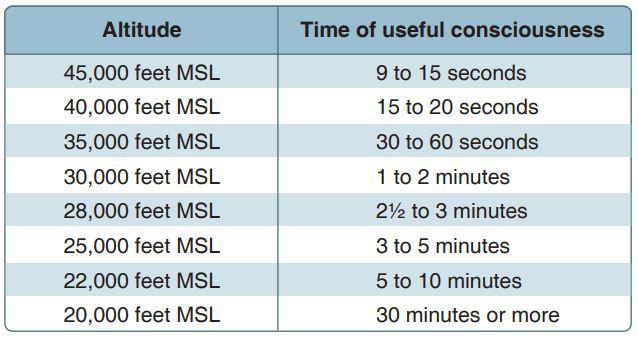
There are four different types of hypoxia. The four types are:
- Hypoxic hypoxia
- Lack of oxygen available to the lungs
- Remedy: descend or use supplemental oxygen or both.
- Hypemic hypoxia
- Blood not able to bind to and transport oxygen from lungs to the rest of your body. Most commonly CO poisoning for pilots
- Remedy: turn off heaters, open air vents, descend and use supplemental oxygen
- Stagnant hypoxia
- Stagnant means the blood is not flowing and transporting oxygen, an example of this could be high G-forces
- Remedy: Do not do aerobatics without lots of proper training and proper equipment
- Histotoxic hypoxia
- The inability of the tissue to use the oxygen in the blood, due to drugs or alcohol
- Remedy: only use approved drugs and do not fly with any alcohol in your system. Do not allow passengers on board your aircraft who are impaired by any drug or alcohol.
The signs of hypoxia are:
- euphoric feeling
- blue fingertips and lips
- slurring of speech
- headache
- slowed response time
- Lightheaded or dizzy sensation
- Tingling in fingers and toes
Hyperventilation
This is when you have too little carbon dioxide in your blood. This could be due to breathing rapidly in a panic (hyperventilating). The remedy is to slow your breathing and possible breath into a paper bag to restore the proper balance of oxygen and CO2 in your system. The signs of hyperventilation aside from a noticeably high breathing rate are:
- Visual impairment
- Unconsciousness
- Lightheaded or dizzy sensation
- Tingling sensations
- Hot and cold sensations
- Muscle spasms
As you can see, the signs are similar to Hypoxia (lack of oxygen). It is important for a pilot to correctly diagnose what they are experiencing so they can act accordingly. If left unchecked, Hyperventilation can lead to unconsciousness as that is the body’s natural defense mechanism to restore the proper balance of CO2 and oxygen in the blood.
Middle ear and sinus problems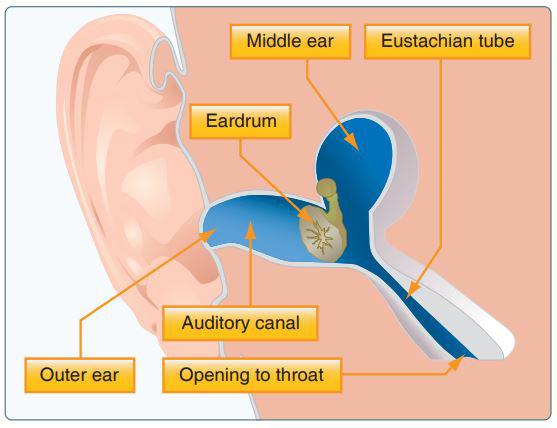
Due to the design of your ear as pictured on the left, it is easier for air to escape than it is for air to re-enter into the ear. The Eustachian tube can help with this. It is the action of swallowing that can help you to equalize the pressure on both sides of your eardrum as the pressure changes during climbs and descents. Because the Eustachian tube is connected to the throat, swallowing or yawning can often help to open the tube and equalize pressure, relieving any pain felt from the differential pressure on your eardrum.
Another less recommended technique (due to the fact you can possibly damage your eardrum doing this) is to hold your nose, close your mouth, and gently exhale, forcing pressure through the Eustachian tube to the middle ear. You might use such a technique when descending and the external pressure on your eardrum is rising.
If a passenger were to complain of ear pain during a descent, you may consider climbing back up to the original altitude, having them equalize their ears there, and continue swallowing and equalizing as you descend again (at a slower rate perhaps too). Ultimately if someone is in excruciating pain as you descend, you can try the prior recommendation, but at some point, you will have to descend and land since you have a limited amount of fuel. Don’t let a problem like a possible ear drum rupturing (that can generally heal on its own over time) cause you to become distracted, run out of fuel, and crash killing yourself, your passenger, and people on the ground. Not all outcomes are great when you have problems in the air, use your ADM skills to get the best possible outcome, it may not always be a wonderful outcome.
Motion sickness
Motion sickness, or airsickness, is caused by the brain receiving conflicting messages about the state of the body. A pilot may experience motion sickness during initial flights, but it generally goes away within the first few lessons. Anxiety and stress, which may be experienced at the beginning of flight training, can contribute to motion sickness.
Remedy: If symptoms of motion sickness are experienced during a lesson, opening fresh air vents, focusing on objects outside the airplane, and avoiding unnecessary head movements may help alleviate some of the discomfort. Although medications like Dramamine can prevent airsickness in passengers, they are not recommended while flying since they can cause drowsiness and other problems.
Carbon monoxide poisoning
CO is a colorless and odorless gas produced by all internal combustion engines. Attaching itself to the hemoglobin in the blood about 200 times more easily than oxygen, CO prevents the hemoglobin from carrying oxygen to the cells, resulting in hypemic hypoxia. The body requires up to 48 hours to dispose of CO. If severe enough, the CO poisoning can result in death. Aircraft heater vents and defrost vents may provide CO a passageway into the cabin, particularly if the engine exhaust system has a leak or is damaged. If a strong odor of exhaust gases is detected, assume that CO is present. However, CO may be present in dangerous amounts even if no exhaust odor is detected. Disposable, inexpensive CO detectors are widely available. In the presence of CO, these detectors change color to alert the pilot of the presence of CO.
Signs: of CO poisoning are headache, blurred vision, dizziness, drowsiness, and/or loss of muscle power.
Remedy: Any time a pilot smells exhaust odor, or any time these symptoms are experienced, immediate corrective action should be taken including turning off the heater, opening fresh air vents and windows, and using supplemental oxygen, if available. Tobacco smoke also causes CO poisoning. Smoking at sea level can raise the CO concentration in the blood and result in physiological effects similar to flying at 8,000 feet. Besides hypoxia, tobacco causes diseases and physiological debilitation that can be medically disqualifying for pilots.
Stress and Fatigue
Stress is the body’s response to physical and psychological demands placed upon it. The body’s reaction to stress includes releasing chemical hormones (such as adrenaline) into the blood and increasing metabolism to provide more energy to the muscles. Blood sugar, heart rate, respiration, blood pressure, and perspiration all increase. The term “stressor” is used to describe an element that causes an individual to experience stress. Examples of stressors include physical stress (noise or vibration), physiological stress (fatigue), and psychological stress (difficult work or personal situations). Stress falls into two broad categories: acute (short-term) and chronic (long-term). Acute stress involves an immediate threat that is perceived as danger. This is the type of stress that triggers a “fight or flight” response in an individual, whether the threat is real or imagined. Normally, a healthy person can cope with acute stress and prevent stress overload. However, ongoing acute stress can develop into chronic stress. Chronic stress can be defined as a level of stress that presents an intolerable burden, exceeds the ability of an individual to cope, and causes individual performance to fall sharply. Unrelenting psychological pressures, such as loneliness, financial worries, and relationship or work problems can produce a cumulative level of stress that exceeds a person’s ability to cope with the situation. When stress reaches these levels, performance falls off rapidly. Pilots experiencing this level of stress are not safe and should not exercise their airman privileges. Pilots who suspect they are suffering from chronic stress should consult a physician.
Fatigue is frequently associated with pilot error. Some of the effects of fatigue include degradation of attention and concentration, impaired coordination, and decreased ability to communicate. These factors seriously influence the ability to make effective decisions. Physical fatigue results from sleep loss, exercise, or physical work. Factors such as stress and prolonged performance of cognitive work result in mental fatigue. Like stress, fatigue falls into two broad categories: acute and chronic. Acute fatigue is short term and is a normal occurrence in everyday living. It is the kind of tiredness people feel after a period of strenuous effort, excitement, or lack of sleep. Rest after exertion and 8 hours of sound sleep ordinarily cures this condition.
A special type of acute fatigue is skill fatigue. This type of fatigue has two main effects on performance:
Timing disruption—appearing to perform a task as usual, but the timing of each component is slightly off. This makes the pattern of the operation less smooth because the pilot performs each component as though it were separate, instead of part of an integrated activity.
Disruption of the perceptual field—concentrating attention upon movements or objects in the center of vision and neglecting those in the periphery. This is accompanied by loss of accuracy and smoothness in control movements.
Acute fatigue has many causes, but the following are among the most important for the pilot:
- Mild hypoxia (oxygen deficiency)
- Physical stress
- Psychological stress
- Depletion of physical energy resulting from psychological stress
- Sustained psychological stress
Sustained psychological stress accelerates the glandular secretions that prepare the body for quick reactions during an emergency. These secretions make the circulatory and respiratory systems work harder, and the liver releases energy to provide the extra fuel needed for brain and muscle work. When this reserve energy supply is depleted, the body lapses into generalized and severe fatigue.
Acute fatigue can be prevented by proper diet and adequate rest and sleep. A well-balanced diet prevents the body from needing to consume its own tissues as an energy source. Adequate rest maintains the body’s store of vital energy.
Chronic fatigue, extending over a long period of time, usually has psychological roots, although an underlying disease is sometimes responsible. Continuous high-stress levels produce chronic fatigue. Chronic fatigue is not relieved by proper diet and adequate rest and sleep and usually requires treatment by a physician. An individual may experience this condition in the form of weakness, tiredness, palpitations of the heart, breathlessness, headaches, or irritability. Sometimes chronic fatigue even creates stomach or intestinal problems and generalized aches and pains throughout the body. When the condition becomes serious enough, it leads to emotional illness.
If suffering from acute fatigue, stay on the ground. If fatigue occurs while you are flying, no amount of training or experience can overcome the detrimental effects. Getting adequate rest is the only way to prevent fatigue from occurring. Avoid flying without a full night’s rest, after working excessive hours, or after an especially exhausting or stressful day. Pilots who suspect they are suffering from chronic fatigue should consult a physician and not fly until properly rested.
Dehydration and nutrition
Dehydration is the term given to a critical loss of water from the body.
Common signs of dehydration are headache, fatigue, cramps, sleepiness, and dizziness. The first noticeable effect of dehydration is fatigue, which in turn makes top physical and mental performance difficult, if not impossible. Flying for long periods in hot summer temperatures or at high altitudes increases the susceptibility to dehydration because these conditions tend to increase the rate of water loss from the body. To help prevent dehydration, drink two to four quarts of water every 24 hours. Since each person is physiologically different, this is only a guide. Most people are aware of the eight-glasses-a-day guide: If each glass of water is eight ounces, this equates to 64 ounces, which is two quarts. If this fluid is not replaced, fatigue progresses to dizziness, weakness, nausea, tingling of hands and feet, abdominal cramps, and extreme thirst. The key for pilots is to be continually aware of their condition. Most people become thirsty with a 1.5 quart deficit or a loss of 2 percent of total body weight. This level of dehydration triggers the “thirst mechanism.” The problem is that the thirst mechanism arrives too late and is turned off too easily. A small amount of fluid in the mouth turns this mechanism off and the replacement of needed body fluid is delayed. Other steps to prevent dehydration include:
- Carrying a container in order to measure daily water intake.
- Staying ahead—not relying on the thirst sensation as an alarm. If plain water is not preferred, add some sport drink flavoring to make it more acceptable.
- Limiting daily intake of caffeine and alcohol (both are diuretics and stimulate increased production of urine).
Nutrition is important for obvious reasons. When you do not have the proper diet, many of your physical functions will suffer. A common trap for pilots to fall into is not eating regularly due to trying to complete flights on a certain time schedule (due to weather or any other reason). If you do not eat, your blood sugar level immediately suffers and your cognitive ability and motor skills will start to suffer, similar if you were suffering from fatigue. Eat regularly and keep snack bars in your flight bag as a backup plan!
Hypothermia
Winter time flying can be beautiful, but there are certain things you need to consider:
- Dress very warm for preflights so you do not rush your preflight being cold
- Ensure you have warm clothes on or at least with you when flying. Just because the airplane is heated you do not want to be forced to land somewhere remote and freeze due to not having proper clothes.
- Recognize the signs and symptoms of hypothermia if you are flying in an airplane that is very cold, i.e. there is no heat available due to old leaky exhaust manifolds.
Dissolved Nitrogen in the Bloodstream After Scuba Dives
Scuba diving subjects the body to increased pressure, which allows more nitrogen to dissolve in body tissues and fluids. The reduction of atmospheric pressure that accompanies flying can produce physical problems for scuba divers. A pilot or passenger who intends to fly after scuba diving should allow the body sufficient time to rid itself of excess nitrogen absorbed during diving. If not, DCS (decompression sickness) due to evolved gas can occur during exposure to low altitude and create a serious in-flight emergency. The recommended waiting time before going to flight altitudes of up to 8,000 feet is at least:
- 12 hours after diving that does not require controlled ascent (nondecompression stop diving)
- 24 hours after diving that does require controlled ascent (decompression stop diving).
The waiting time before going to flight altitudes above 8,000 feet should be at least 24 hours after any scuba dive. These recommended altitudes are actual flight altitudes above mean sea level (MSL) and not pressurized cabin altitudes. This takes into consideration the risk of decompression of the aircraft during flight.
